What Is Incontinence Dermatitis
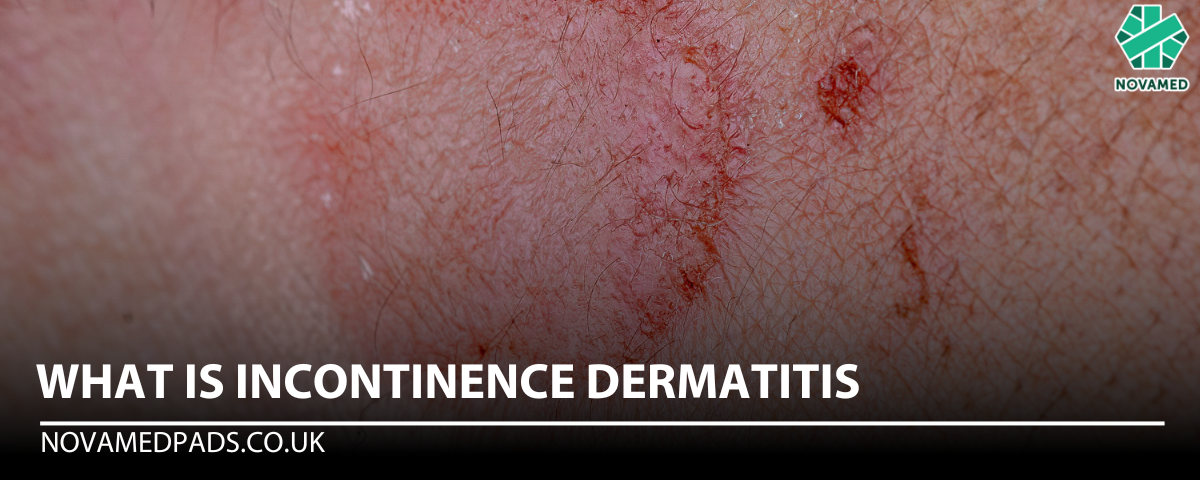
Incontinence dermatitis, also known as moisture-associated skin damage (MASD), is an inflammation of the skin caused by prolonged exposure to urine or stool. This condition typically leads to redness, flaking, irritation, and discomfort. It most commonly occurs in areas of the body prone to moisture and friction, such as the groin, lower back, under the breasts, and armpits.
Common Causes of Incontinence Dermatitis
Incontinence dermatitis is frequently found in individuals who suffer from urinary or faecal incontinence. The condition worsens when tight-fitting clothing traps heat and moisture, leading to further skin irritation. When heated urine remains in contact with the skin for extended periods, it can cause blisters and dryness, leading to scaly patches known as ichthyosis digitiform (characterised by a fish-scale appearance).
Prevalence and Risk Factors
Although there is no precise data on how many people are affected by incontinence dermatitis, it is a common condition among those with urinary incontinence. Women are often more affected due to their tendency to wear tight-fitting clothing, which increases the likelihood of trapping moisture and irritating the skin.
How to Prevent Incontinence Dermatitis
While incontinence dermatitis cannot be entirely prevented, it can be managed effectively through proper care. Below are some steps to reduce the risk:
- Use absorbent pads or undergarments: These help retain urine and stool, reducing contact with the skin and preventing irritation.
- Change incontinence products frequently: Always follow the manufacturer's instructions, changing the products more often if there are signs of irritation or risk of skin breakdown.
- Avoid tight-fitting clothing: Clothing that traps heat and moisture, such as leotards or overly tight underwear, can exacerbate the condition. Opt for clothing that allows the skin to breathe.
- Good skincare hygiene: Regularly cleanse and dry the skin, changing clothes and bed linen when they become damp or soiled.
Treatment for Incontinence Dermatitis
Several treatment options are available for incontinence dermatitis, ranging from topical treatments to lifestyle adjustments. Some common treatments include:
1. Topical Products
Topical treatments, such as those containing triclosan or ketoconazole, can help manage inflammation and fungal infections. Triclosan has anti-inflammatory and antifungal properties but may increase the risk of contact dermatitis in individuals with allergies. On the other hand, ketoconazole is an effective antifungal agent that can be applied to the skin, though it has not been shown to prevent other types of skin infections.
2. High-Power Laser Therapy
For individuals with more severe cases, high-power laser therapy may help reduce the symptoms of incontinence dermatitis. While those with mild cases may not experience significant improvement, this therapy has shown promising results in more severe cases.
3. Over-the-Counter and Natural Products
Many over-the-counter and natural products can help alleviate symptoms. These products often contain ingredients such as tea tree oil, neem leaf extract, or balsam fir needle oil, known for their soothing and anti-inflammatory properties. They can be found in most pharmacies or health shops.
Best Practices for Managing Incontinence Dermatitis
The key to managing incontinence dermatitis lies in proactive skincare and lifestyle changes. Some recommendations include:
- Maintain a healthy diet: A balanced diet can improve overall skin health and help prevent infections.
- Avoid harsh skincare products: Do not use products like baby powder or perfumed shower gels, which can worsen the irritation. Instead, opt for talc-free powders and mild cleansers.
- Regular bathing: Regularly cleanse the affected areas with gentle soap and water to keep the skin free from irritants.
Related Conditions: Ichthyosis
Ichthyosis, a hereditary skin condition, shares similar symptoms with incontinence dermatitis, such as dry, scaly skin. It can range from mild to severe and occurs in all races. There are various types of ichthyosis, including:
- Ichthyosiform erythroderma: A waxy type of ichthyosis.
- Keratoderma blennorrhagicum: A blistering form.
- Scleritis-ichthyosis: A symmetrical form.
One of the first treatments for ichthyosis is a regular bath using special soap to prevent the skin from drying out and cracking.
Final Thoughts
Incontinence dermatitis can be an uncomfortable and persistent condition, but with the right care and lifestyle adjustments, it can be managed effectively. If you suspect you may be developing symptoms of this condition, consult with a healthcare professional for tailored advice on the best treatment and prevention strategies.
Feel free to explore our full range of incontinence solutions here!
Bladder and bowel incontinence may be caused by conditions which can be treated medically. Please consult your physician for medical advice and guidance.




